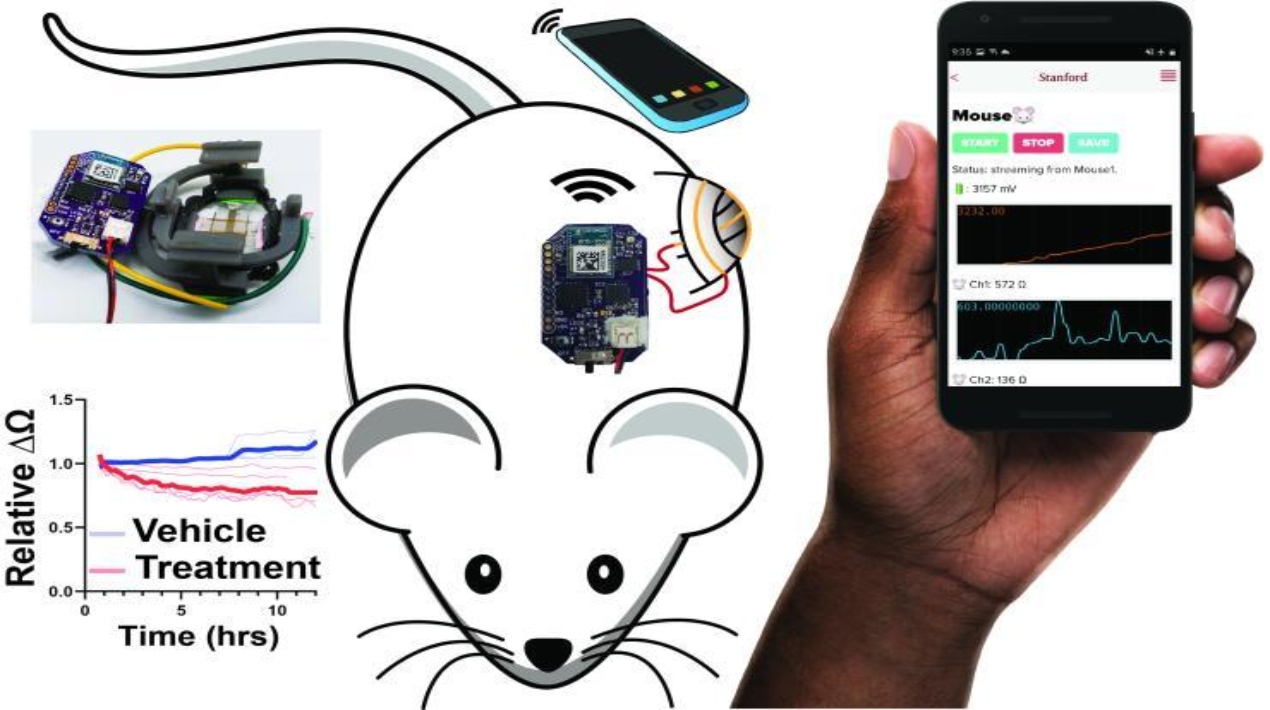
A compact, autonomous gadget with a flexible sensor that can be attached to the skin has been developed by engineers at the Georgia Institute of Technology along with Stanford University to measure the changing size of tumours beneath the skin.
The battery-operated, non-invasive device is sensitive to one-hundredth of a millimetre (10 micrometres) and can wirelessly transmit results to a smartphone app in real-time at the touch of a button.
According to the researchers, the device tag FAST short for Flexible Autonomous Sensor measuring Tumours represents an entirely novel, affordable, hands-free, and accurate method for testing the efficiency of anti-cancer medications. On a larger scale, it could lead to promising new cancer treatment possibilities.
Researchers test thousands of potential cancer treatments on mice with subcutaneous tumours each year. Few make it to human patients, and the process of discovering novel medicines is sluggish since technologies for evaluating the shrinkage of tumours in response to medication therapy require weeks to determine a response.
The inherent biological heterogeneity of tumours, the limitations of existing measurement methods, and the relatively small sample sizes make medication tests challenging and laborious.
Metal pincer-like callipers are not appropriate for measuring soft tissues, and radiological techniques cannot provide the continuous data required for real-time assessment. While calliper and bioluminescence tests frequently need weeks-long observation periods to read out changes in tumour size, FAST can detect changes in tumour volume on a minute-timescale.
The FAST sensor is comprised of a skin-like, elastic polymer with an embedded layer of gold circuitry. This sensor is attached to a small electronic backpack designed by Yasser Khan and Naoji Matsuhisa, two former post-docs and co-authors.
The device monitors the membrane’s strain, or how much it stretches or contracts, and transfers this information to a smartphone. Using the FAST backpack, possible therapies connected to tumour size reduction can be promptly and confidently ruled out as useless or expedited for further investigation.
According to the experts, the new device offers at least three substantial improvements. First, it allows continuous monitoring because the sensor is physically attached to the mouse and remains in place during the duration of the experiment.
Second, the flexible sensor envelops the tumour and is consequently able to measure difficult-to-detect changes in form that cannot be detected by other methods. FAST is autonomous and non-invasive. It is affixed to the skin like a bandage, is battery-powered and wirelessly connected.
Following sensor placement, the mouse is unconstrained by the gadget or wires and scientists are not required to actively touch the mice. FAST packs are also reusable, cost approximately $60 to assemble, and can be connected to a mouse in a matter of minutes.
The breakthrough is the flexible electronic material developed by FAST. The skin-like polymer is coated with a coating of gold, which, when stretched, generates microscopic fissures that alter the material’s electrical conductivity.
Stretching the material increases the number of cracks, which in turn raises the electrical resistance of the sensor. When the material compresses, the cracks reconnect, and conductivity is enhanced. Researchers defined how fracture propagation and exponential changes in conductivity might be theoretically linked to dimensional and volumetric changes.
The researchers had to overcome the risk that the sensor itself could skew results by providing excessive pressure on the tumour, thereby compressing it. To avoid this danger, they meticulously matched the mechanical properties of the flexible material to those of skin, making the sensor as malleable and pliable as actual skin.
















